Eye Conditions

Corneal Abscess in the Horse
The cornea is the clear front part of the eye. A thin layer of tissue called epithelium is the cornea’s protective outer layer. The inner surface is called the endothelium and the portion in between is called the stroma. A corneal abscess occurs when bacteria or fungus along with the animal’s own white blood cells enter the cornea through an injury. The injury may heal too quickly and essentially “seal” the bacteria or fungus inside the cornea creating a pocket of infection or abscess. Abscesses may also be sterile, with only white blood cells present.
A horse with a corneal stromal abscess will have a dense white or yellow spot in the cornea representing an accumulation of organisms (bacteria or fungi) and/or white cells. The eye may be cloudy and red with varying levels of ocular discomfort, which may manifest as tearing and squinting of the affected eye. A corneal stromal abscess may weaken the cornea to the point of perforation of the eye, with the possibility of subsequent blindness. It is also possible that the abscess may spread to the inside of the eye causing severe intraocular inflammation and infection, which also may be vision-threatening.
Corneal stromal abscesses are treated intensively with medications prescribed by the veterinary ophthalmologist. The ophthalmologist may remove the corneal epithelium covering the abscess to increase penetration of medication into the lesion to hasten the healing process. Medications may need to be continued for several weeks to several months. Surgical intervention is occasionally necessary to remove the organisms (bacteria or fungi) and prevent rupture of the eye. These surgeries can vary depending on the depth of the abscess and occasionally utilize a corneal or conjunctival graft to cover the surgical site. These grafts incorporate into the cornea at the site of the abscess forming a dense scar in a few weeks. The goal is to preserve the vision and globe by provide structural support to the cornea and bring in blood supply to facilitate healing to the weakened and diseased tissue. Healing of a corneal stromal abscess with or without surgery will result in a scar on the cornea. The size and location of the scar will dictate the degree of vision impairment (if at all). The performance of your horse may or may not be affected by the corneal scar.
While treating for a corneal stromal abscess, the horse should be kept in a darkened stall with limited exercise. Hay should be removed from overhead racks and fed on the ground. An Eye Saver Mask can be used to protect the eye self-trauma and from fly strike. In many cases, frequent medication application can be performed with ease by the placement of a subpalpebral lavage system. Please speak to your veterinarian or veterinary ophthalmologist if you are interested in having a subpalpebral lavage system placed.
If you have any further questions or concerns regarding corneal abscesses, please do not hesitate to call us at Eye Care for Animals.
Less Info
Equine Cataracts
By definition, a cataract is an opacity of the lens that obstructs passage of light and impedes vision. A cataract may appear as cloudiness or haze in your horse’s eye. Cataracts can develop for a variety of reasons and some types will cause more severe vision impairment than others. Cataracts can also lead to secondary complications, such as glaucoma – a painful eye condition. A horse may be born with cataracts (congenital cataracts), develop them at a young age (juvenile cataracts), or develop them as an adult. In general, this is an uncommon condition in the horse.
Congenital and juvenile cataracts are believed to be due to either hereditary condition or an abnormality during development inside the mare. This type of cataract is fortunately quite rare in horses. The possible hereditary nature of this type of cataract should be taken into consideration when breeding these horses and their close relatives.
The majority of cataracts in horses occur in adult animals. They most commonly develop secondary to diseases that cause intraocular inflammation, such as Equine Recurrent Uveitis (ERU, moon blindness). The second most common cause of equine cataract is trauma – both blunt and sharp trauma. All eye injuries should be evaluated by a veterinarian at the time of injury, as well as, at future rechecks to monitor for development of cataract.
The management of equine cataracts depends on the type and size of cataract present, as well as, the intended use of the horse. Cataracts that remain small enough that vision is not significantly impaired may not require treatment or require topical medical treatment only. A complete or mature cataract may be a surgical candidate. No medication will dissolve cataracts and cataracts are only resolved by surgical removal. Some equine cataracts can be removed by phacoemulsification and replaced by an intraocular lens, but this surgery is not an option for all horses. An in-depth discussion with a veterinary ophthalmologist can help to determine if your horse is a possible candidate. Foals with congenital or juvenile cataracts may benefit from early cataract removal surgery and have improved surgical outcomes. This higher rate of success is due to the smaller size of the foal eye and the decreased association between inflammation and cataract in foals.
The success rate for congenital/juvenile equine cataracts is approximately 85% in terms of vision while that for adult horses with acquired cataracts may be much less. Success rates for adult horses vary depending on the cause of cataract, chronicity, and any underlying disease. For instance, the surgical outcome for traumatically-induced cataracts in adults is highly favorable, while outcome for cataracts from chronic ERU is guarded (50% or even less chance of maintaining vision long-term).
Potential complications of lens removal in the horse may include: persistent or recurring intraocular inflammation, corneal ulcers, corneal cloudiness or edema, loss of vision, glaucoma, and retinal detachment. Leaving the cataract in the eye, unfortunately, has many of the same possible complications. While cataracts are not painful, many of these complications can cause discomfort and/or blindness.
Pre- and post-operative treatment should be discussed as well. If surgical removal is being considered, pre-surgical diagnostic testing is recommended prior to cataract surgery, including an ocular ultrasound and electroretinogram to evaluate retinal function and integrity.
Post-operative treatment should also be a consideration. Medical treatment with topical and oral medications for a month or longer may be required following the procedure to maximize chances of success. Immediately after surgery, medications will be given multiple times per day via a subpalpebral lavage system. Your horse should also wear a protective mask (Eye-Saver) for days to a week after surgery. During the post-operative treatment period, your horse may need to be kept out of bright light and will have marked exercise restrictions.
It is important to realize that a horse with an intraocular lens and a successful surgery is not considered to have normal vision. Fortunately, most horses seem to adapt quite well and are capable of returning to pre-surgical work. If a lens is not placed, your horse will be “far-sighted,” meaning the “close up” vision is poor. It is important that your horse be considered visually impaired and you, as the owner, are responsible for the safety of any other riders you allow on your horse. That said, many owners of visually impaired horses find them to be wonderful companions and athletic partners.
If you have any further questions or concerns about equine cataracts, please do not hesitate to call us at Eye Care for Animals.
Less Info
Equine Corneal Ulcers
The cornea is the clear dome-shaped structure that forms the front surface of the eye. It allows light to enter the eye and helps to focus it on the retina for functional vision. It also protects the structures inside the eye and maintains ocular shape and integrity. A corneal ulcer is simply a break on the surface of the cornea and leads to loss of the outer layer or epithelial surface of the eye. Ulcers have many possible causes: trauma, lacerations, abrasions, drying due to abnormal tear production, eyelid abnormalities, foreign material, parasites, viral infections, insect stings, chemical sprays or inflammation, intraocular disease, etc. Often the initial cause cannot be determined but treatment is similar for most corneal ulcers, as they are essentially open wounds on the eye. Signs of ulceration include squinting, tearing, discomfort, watery or mucoid discharge, redness and sensitivity to light. Cloudiness of the cornea or discoloration may also be noted.
A superficial, uncomplicated ulcer usually heals uneventfully in about 1 week with minimal scarring after appropriate medical treatment. A corneal ulcer can become secondarily infected with bacteria, fungi, or a mixture of the two. Infected, deep, or complicated ulcers require more intensive medical treatment and sometimes surgery. Corneal ulcers should be evaluated by a veterinarian. In addition to the exam, the veterinarian may take samples of the ulcer for cytology, bacterial and/or fungal culture. These tests will help determine the most appropriate therapy.
In complicated cases, the ulcer may rapidly deepen or the cornea may start a breakdown process called “melting”. A “melting” cornea can even progress to rupture of the eye. Melting and deep ulcers are considered eye emergencies. Secondary inflammation, or uveitis inside the eye, is painful and can contribute to vision-threatening complications. The ulcer may require intensive, frequent treatments for several days to weeks to control infection, reduce melting and control inflammation in order to achieve healing and save the globe. Deep and complicated corneal ulcers generally result in more noticeable scarring after healing. Large or dense white scars can cause visual impairment and the horse’s athletic performance or intended use may be affected.
Deep or melting ulcers that worsen despite therapy may require surgery in addition to medical therapy to save the eye. These surgeries usually involve grafting of additional supportive tissue or biosynthetic material, such as a flap of conjunctiva (tissue from the “pink” part of the eye), into the ulcer. This helps to fill in the tissue defect, bring in a blood supply, and hasten healing. These grafts usually incorporate into the corneal tissue in a few weeks to months but also may result in a permanent scar.
If you have any further questions or concerns regarding equine corneal ulcers, please do not hesitate to call us at Eye Care for Animals.
Less Info
Equine Recurrent Uveitis
Uveitis means inflammation of the iris and deeper structures inside the eye. Equine recurrent uveitis (ERU) is the most common cause of defective vision or blindness in the horse. ERU is also known as “periodic ophthalmia” and “moon blindness”. It is characterized by multiple episodes of “active” uveitis alternating with periods when the eye is “quiet”, or not inflamed. One or both eyes may be involved in the disease. Chronic ERU may result in partial or complete loss of vision. Signs of “active” ERU include tearing, squinting, sensitivity to light, and a cloudy or red eye. The active episodes of ERU cause permanent changes in the eye, including scarring of parts of the eye and possibly cataracts or retinal detachments. These permanent changes can be seen by a veterinary ophthalmologist even during the “quiet” stages of the disease. During the “quiet” stages, the eye is not painful and inflammation is minimal. ERU is caused by an overly active immune response of the eye to many different sources. The source may be bacterial (such as Leptospira, Brucella, Salmonella, or Streptococcus), viral, parasitic (such as Onchocerca, Strongylus, or Toxoplasma), or fungal. Trauma to the eye or certain diseases of the body can also be sources of ERU. It is important to remember that the source only initiates ERU. The original source may be treated or may go away, but the horse’s own immune system may perpetuate the inflammation and disease in the eye. Relapses of inflammation may continue to occur although the original source of inflammation is no longer there. Identifying the original source of inflammation may prove to be very difficult, and in many cases, the causative agent or original source of inflammation is never identified. A genetic predisposition to ERU as some breeds, such as Appaloosas, which have a higher incidence of the disease, may exist.
Treatment of ERU alleviates the pain associated with the “active” stages of the disease and decreases inflammation in the eye while also attempting to preserve vision. Medications should be prescribed by your veterinarian as soon as signs of ERU are noted. For each “active” stage of the disease, it may be necessary to continue treatment of the eye for several weeks to several months, depending on the severity of inflammation. Although most treatment involves a combination of topical eye drops/ointment and oral or injectable medications, some patients may be candidates for a surgical implant device that slowly releases cyclosporine, an immunomodulatory medication.
Relapses of inflammation of the eye require reinstatement of topical and systemic treatment by your veterinarian. It is important to contact your veterinarian or veterinary ophthalmologist if you feel your horse is having a recurrence of ERU. Signs of ERU can be similar to other conditions such as glaucoma or corneal ulceration and some of the medications used to treat ERU may be contraindicated for these conditions. Thus, it is important that you consult your veterinarian or veterinary ophthalmologist prior to restarting medications for ERU. It is also important that you contact your veterinary ophthalmologist prior to stopping or decreasing the frequency of any prescribed medications. It is helpful to keep the horse in a darkened stall with limited exercise during treatment periods. If treatment fails and the eye becomes blind and painful, the eye may need to be removed to eliminate discomfort.
The prognosis for vision in horses affected with ERU can be poor. Prompt treatment may slow or prevent the occurrence of blindness.
If you have any questions regarding equine recurrent uveitis or any other eye condition, please do not hesitate to call us at Eye Care for Animals.
Less Info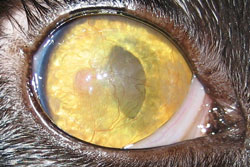
Proliferative Keratoconjuntivitis (Eosinophilic Keratitis)
Eosinophilic keratitis is an inflammatory condition that affects the cornea and/or conjunctiva. The characteristic appearance is white, tan or pink roughened plaques on the corneal surface. These plaques are composed of inflammatory cells known as eosinophils. The cause of eosinophilic keratitis is believed to be related to an underlying feline herpesvirus infection. This disease is progressive and can grow to involve the entire surface of the eye causing blindness and discomfort. Often it is initially detected in one eye; however, the disease often progresses to involve both eyes.
Superficial corneal scraping is usually adequate to obtain a diagnosis, which is confirmed by the presence of eosinophils under light microscopy. Occasionally, microscopic examination is not sufficient for diagnosis and further diagnostics may be recommended.
Due to its suspected association with feline herpes virus (FHV-1), diagnostic testing and/or empirical treatment for herpes virus may also be indicated. Treatment for eosinophilic keratoconjunctivitis consists of topical anti-inflammatory medications and/or systemic hormonal modification. Ovaban (megestrol acetate) is a synthetic progesterone (hormone) used to treat this disease. It is very effective but does have possible side effects, which may include transient diabetes mellitus, enlargement or (rarely) cancer of the mammary gland, and liver toxicity. The length of treatment is variable and some cats may have disease recurrence when medications are discontinued. The majority of patients can remain comfortable and visual when there is client compliance with respect to the medication schedule.
If you have any questions or concerns regarding Eosinophilic Keratitis, please call Eye Care for Animals.
Less Info
Squamous Cell Carcinoma
Squamous cell carcinoma is one of the most common periocular tumors in horses, specifically horses located in areas of intense sunlight or high altitude. Non-pigmented regions of the skin are susceptible to the development of this tumor. The tumor may involve the eyelids, third eyelid, cornea or the tissues surrounding the eye itself. Appaloosas, color-dilute breeds, Belgians and other draft horses are particularly susceptible to development of this tumor.
A horse with an early squamous cell carcinoma lesion can be seen with a reddening, roughening or ulcerated area, along with increased tearing of the eye. The tumor soon develops into a small pink or red mass, which if left untreated, can enlarge and spread around and behind the eye, to the skull, sinuses of the skull, brain and to other parts of the body. Squamous cell carcinoma can be diagnosed in its earliest stages by a biopsy of the lesion, which can be performed by your veterinarian or veterinary ophthalmologist. Treatment and prognosis of squamous cell carcinoma vary with the location, size, and the extent of the tumor. Treatments may involve surgical removal, freezing or heating, radiation, laser ablation, immunotherapy, chemotherapy or a combination of the above. In some of these cases, the tumor becomes inoperable and the outcome can be devastating. There is potential for recurrence of the tumor despite the type of treatment used, and additional treatments may be necessary. The prognosis for horses with squamous cell carcinoma is usually good if the tumor is small and can be completely excised. If the tumor is large and extensive or involves the eyelids or space behind the eye, the prognosis may be poor.
The following are recommendations to minimize your horse’s risk of squamous cell carcinoma: avoid peak sun exposure between 10 a.m. and 3 p.m.; provide protection of the eyes from insects, dust, and wind by using an ultraviolet protective mask, sunscreen and fly repellent.
If you have any further questions or concerns regarding Squamous Cell Carcinoma, please do not hesitate to call us at Eye Care for Animals.
Less InfoFind a location
New Patients
Prepare for Your Visit:
New Patient FormEquine Client Info Form
Browse Eye Conditions
Referring Doctors
Educational MaterialsVet Referral Form